Smarter administration and smoother operations for improved cash flow management
In 2026, home health agencies must manage order processes that navigate complex administrative requirements and payer protocols. This complexity demands clinical-level precision. Even small errors can jeopardize claims, lower revenue, disrupt continuity of patient care, and even trigger reviews of previously submitted billings.
This article explores the challenges inherent in clinical administrative practices and outlines a strategic plan to enhance operational performance.
Top Five Reasons for administrative complexity in Home Health Clinics
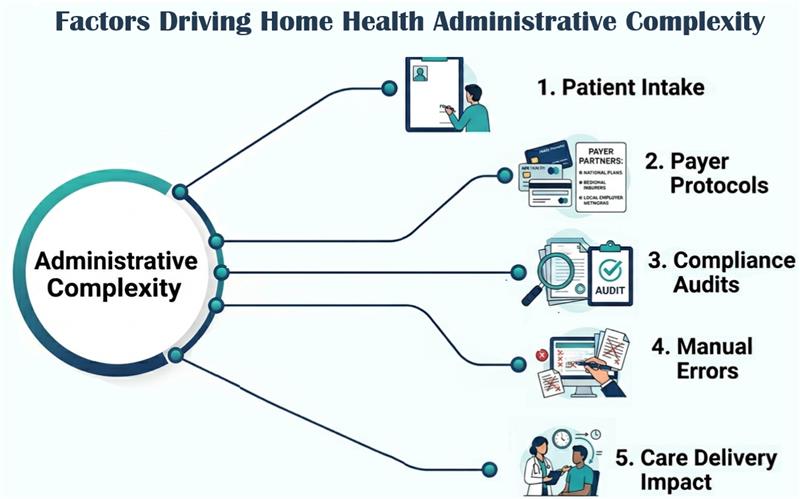
Here are the five primary factors that drive clinical outcomes in home health and hospice.
Patient intake procedure: Efficient patient intake relies on precise documentation and synchronized approvals to meet clinical protocols. Delays at any stage can create bottlenecks across the entire revenue cycle.
Complicated Payer Protocols: Each insurer, especially within the Medicare Advantage (MA) ecosystem, operates with its own unique and frequently updated rules for authorizations, documentation, and submissions.
Strict Compliance Audits: Audits from CMS and other payers have shifted focus from simple signature completion to narrative specificity. A mismatch between a physician’s note and the home health diagnosis can trigger an immediate denial.
High Risk of Manual Error: When staff manually track orders, re-fax documents, and enter data across disconnected systems, the potential for small but costly errors increases dramatically including HIPPA compliance considerations.
Direct Impact on Care Delivery: Administrative delays aren't just a billing concern. A hold-up in obtaining a physician’s order can delay the Start of Care (SOC), prevent a patient from receiving necessary medical equipment, or interrupt a critical treatment plan. Such a delay may even require a separate diagnosis.
Ability to prioritize the right patient: Not all delays affect you equally. Postponing critical paperwork hits your cash flow much faster than delaying smaller tasks. That's why you should always prioritize based on financial risk—not just deadlines.
Without specialized expertise, it might be hard to create fully custom processes to manage a home health or hospice administrative process. In these cases, outsourced home health administrative services could manage operations when specialized expertise is limited.
1. Patient Intake process is getting more challenging
Most home health agencies face delays in the intake of new patients. Here are some of the reasons.
Inconsistencies and gaps in patient referral documentation that require repeated follow-ups
Delays in physician orders, particularly for initial and subsequent certifications
Manual data entry combined with disconnected systems, resulting in duplicated effort and errors
Authorization bottlenecks driven by increasingly strict payer requirements
Communication gaps between intake, clinical, and physician teams
Lack of standardized workflows, leading to inconsistency and unnecessary rework
Here, delays can compound quickly; even a minor bottleneck at intake creates ripples that affect the entire revenue cycle.
2. Following the Payer Protocols by each Insurer
Under the current Value-Based Purchasing (VBP) models, guaranteeing an excellent clinical care doesn’t guarantee patients success. Under the current Medicare Advantage (MA) ecosystem, here are some compliance measures that you should consider.
Claims cannot be submitted without complete and signed orders
Reimbursement timelines are increasingly tied to documentation accuracy and timeliness
Compliance requirements have become stricter, increasing the risk of denials or payment delays
Operational inefficiencies erode margins faster than clinical improvements can offset
3. Undertaking strict Compliance Audits
Most home health agencies mistake a review of the EMR dashboards for an in-depth audit too for visibility. You need to check more than aging orders and unsigned Plans of care but need to take steps to proactively audit and manage their portfolio. Here, the missing authorization, the mismatched code leaves your team to do the same tired manual work they’ve always done, click “re-fax,” resubmit, and hope for the best.
Coding & documentation variance – Even when clinical documentation is correct for one payer, another may deny it as “insufficient” or “not medically necessary” based on their own proprietary guidelines. This leads to rework, delayed payments, and write-offs
Multiple payer portals – Staff must learn different logins, data entry formats, and claim status inquiry methods. This administrative friction directly increases cost-to-collect and reduces time available for patient care or high-value tasks.
Appeal complexity – Payers have different deadlines (e.g., 30 days vs. 180 days), required forms, and levels of appeal. Missing a single deadline or using the wrong form can forfeit legitimate reimbursement.
Prior authorization chaos – Requirements differ by service, setting, and plan even within the same payer. Unexpected denials for missing or “incorrect” auths delay care and create patient dissatisfaction.
Recent audit trends reveal that effective order management requires clinical judgment—not just paperwork—to make sure the physician’s documentation genuinely matches the home health diagnosis.
While mastering all of these administrative capabilities is challenging, an outsourced administrative approach could help you address some of these difficulties.
4. Prioritization of the individual patient care and attention
Every home health agency faces the same daily struggle: a long, endless list of aging physician orders. The default approach seems obvious—start with the oldest and work your way down—but this is a serious error, because not every delay carries the same risk. A three-day hold on a routine supply order is merely an inconvenience, while a 24-hour hold on a Start of Care (SOC) OASIS is a five-alarm crisis threatening your cash flow.
The hidden cost of poor prioritization: when your team chases low-priority paperwork, truly harmful delays fester—DME delays can stall a patient's discharge or recovery, wound care orders introduce serious clinical risk and liability, and SOC OASIS documents directly block billing for an entire episode of care. Think of the SOC OASIS as the ultimate financial threat—no signature, no revenue. Giving it the same attention as a routine follow-up is a losing strategy.
Shift from a to-do list to a triage matrix: instead of sorting by date, top-performing agencies triage work using a simple framework weighing financial impact (high to low) and clinical risk (critical to routine), turning a reactive list into a proactive action plan.
Your new triage workflow for home health
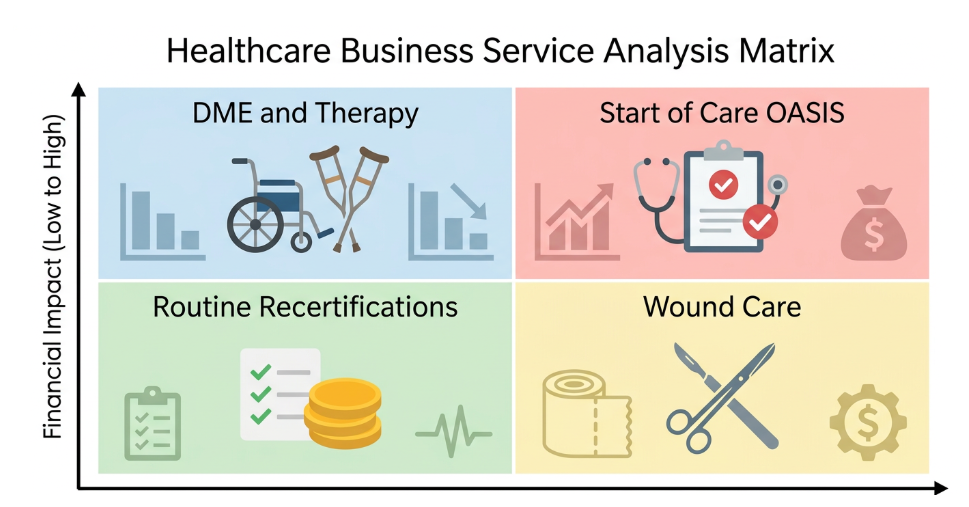
Priority 1—immediate escalation for SOC OASIS, because revenue is frozen until signed;
Priority 2—same-day follow-up for wound care and high-risk clinical orders due to patient safety and liability;
Priority 3—scheduled follow-up within 24-48 hours for DME and therapy orders essential to care progression; and
Priority 4—batch processing for routine recertification and follow-up orders, which carry lower immediate risk. This strategic shift from chronological work to risk-based triage is one of the fastest and most effective ways to improve cash flow and protect your agency—all without adding staff.
5. Creating guard rails against high-risk human errors
A simple human error can completely disconnect the excellent care you provided from the payment you should earn. Here are some ways where the manual can cost you dearly.
A single mistyped digit in a patient ID or date of service can cause an entire claim to be rejected, requiring manual rework.
Discrepancies between clinical notes and billing codes, often from manual data entry, result in pended claims and payment delays.
Manual tracking of authorizations and signed orders inevitably leads to missed deadlines and documentation gaps that auditors can easily flag.
The time staff spends correcting data entry mistakes, resubmitting claims, and chasing down paperwork is a direct and hidden drain on profitability.
A Small in-house team logging into multiple portals and tracking different requirements inevitably leads to inconsistent turnaround times.
Pending Revenue – An Administrative on-hold
If you experience any one of these —or a combination—of the issues listed, it often creates a bottleneck in your revenue cycle. Many home health agencies face held claims due to unsigned orders and backlogged documentation.
These “Pending Revenue” is often just a polite way of saying “Administratively on hold.”
High-level reports may show healthy overall growth, but they rarely reveal the why or how long behind those unpaid claims. These delays demand immediate attention and aggressive follow-up—otherwise, they never reach the bottom line.
Conclusion:- From Administrative Deadlock to Revenue Flow
In the stringent regulatory environment of 2026, clinical excellence is often undermined by administrative roadblocks. Unprocessed orders and documentation backlogs aren't just tedious tasks—they pose a direct risk to your cash flow. When agencies allow these delays to continue, they fall into a "dangerous cycle" where missing signatures drive up days in accounts receivable (AR), leading to unpredictable revenue and shrinking profit margins.
Ultimately, optimizing your revenue cycle goes far beyond administrative upkeep—it is fundamental to your agency's long-term viability. By implementing the strategies detailed in this guide, you can recover valuable staff time, reduce days in accounts receivable, and ensure your financial health reflects the high standard of care you deliver. Don't let administrative backlogs kill your home health agencies momentum. Take action today to seamlessly connect your clinical excellence with the timely reimbursement you deserve.









Recommended Articles
Nov, 2025 Efficient_Revenue_Cycle_Management
Read MoreSep, 2025 Navigating the New HOPE Tool
Read MoreJune, 2025 Preparing for CMS’s All-Payer OASIS Requirement
Read MoreJan, 2025 Home Care Trends to Watch For in 2025
Read MoreDec, 2024 Key Updates in the CY 2025 Home Health Prospective Payment
Read MoreNov, 2024 The Final Rule for Home Health Prospective Payment System
Read MoreOct, 2024 Top Strategies to Maximize Efficiency in Home Health and Hospice Billing
Read MoreSep, 2024 Navigating the 2025 ICD-10-CM Revisions with cliniqon
Read MoreAug, 2024 How Outsourcing Revenue Cycle Management Can Benefit
Read MoreJul, 2024 Update to Review Choice Demonstration: Removal of Choice 3
Read MoreMay, 2024 The Most Common Data Security Threats in Revenue Cycle
Read MoreMarch, 2024 Overcoming the Top 5 Reasons for Denied Home Health Claims
Read MoreFeb, 2026 How Applied Behavior Analysis (ABA) Clinics can better manage their revenue cycle with the right partners
Read MoreFeb, 2026 Why Healthcare Agencies Needs Efficient Medical Coding and Data Auditing Practices
Read MoreFeb, 2026 Eliminating Documentation Burnout...
Read MoreJan, 2026 Eliminating Documentation Burnout...
Read MoreJan, 2024 Addressing Reimbursement Challenges in Home Healthcare
Read MoreDec, 2023 Home Healthcare Trends To Watch For In 2024
Read MoreNov, 2023 CMS Update: Expansion of Review Choice Demonstration for Home
Read MoreOct, 2023 Enhancing Denial Management on Home Healthcare Claims
Read MoreSep, 2023 Cost-Effective Solutions: How Outsourcing is Reshaping Home
Read MoreJul, 2023 Impact of Staffing Shortages on Home Health Agencies
Read MoreMay, 2023 OASIS-E Changes and its Impact on Home Health Agencies.
Read More